
10 Essential Features of Medical Billing Electronic Claims Software
Introduction
In an increasingly complex healthcare landscape, the efficiency of medical billing processes is crucial to a practice's financial health. Medical billing electronic claims software presents a solution that enables providers to streamline operations, reduce errors, and enhance patient satisfaction. However, with a multitude of features available, it is essential to identify the key elements that can elevate a practice’s revenue cycle management. By exploring the ten critical features of this software, we can uncover not only the benefits but also the challenges healthcare providers encounter in optimizing their billing processes.
Automated Claim Submission
Medical billing electronic claims software allows healthcare providers to electronically submit claims to insurance payers without the need for manual intervention. This feature significantly minimizes errors linked to manual data entry and expedites the claims process, resulting in reimbursements that are typically 15-25% faster, based on our clients' experiences. By automating this step, practices can alleviate administrative burdens, allowing staff to focus more on client interactions and care. This increased efficiency, facilitated by medical billing electronic claims software, also leads to a 20-30% reduction in claim denials, thereby enhancing overall satisfaction through clearer billing processes. Furthermore, the automated claim submission process encompasses denial management and appeals, ensuring that underpaid or denied claims are addressed effectively.
Real-Time Eligibility Verification
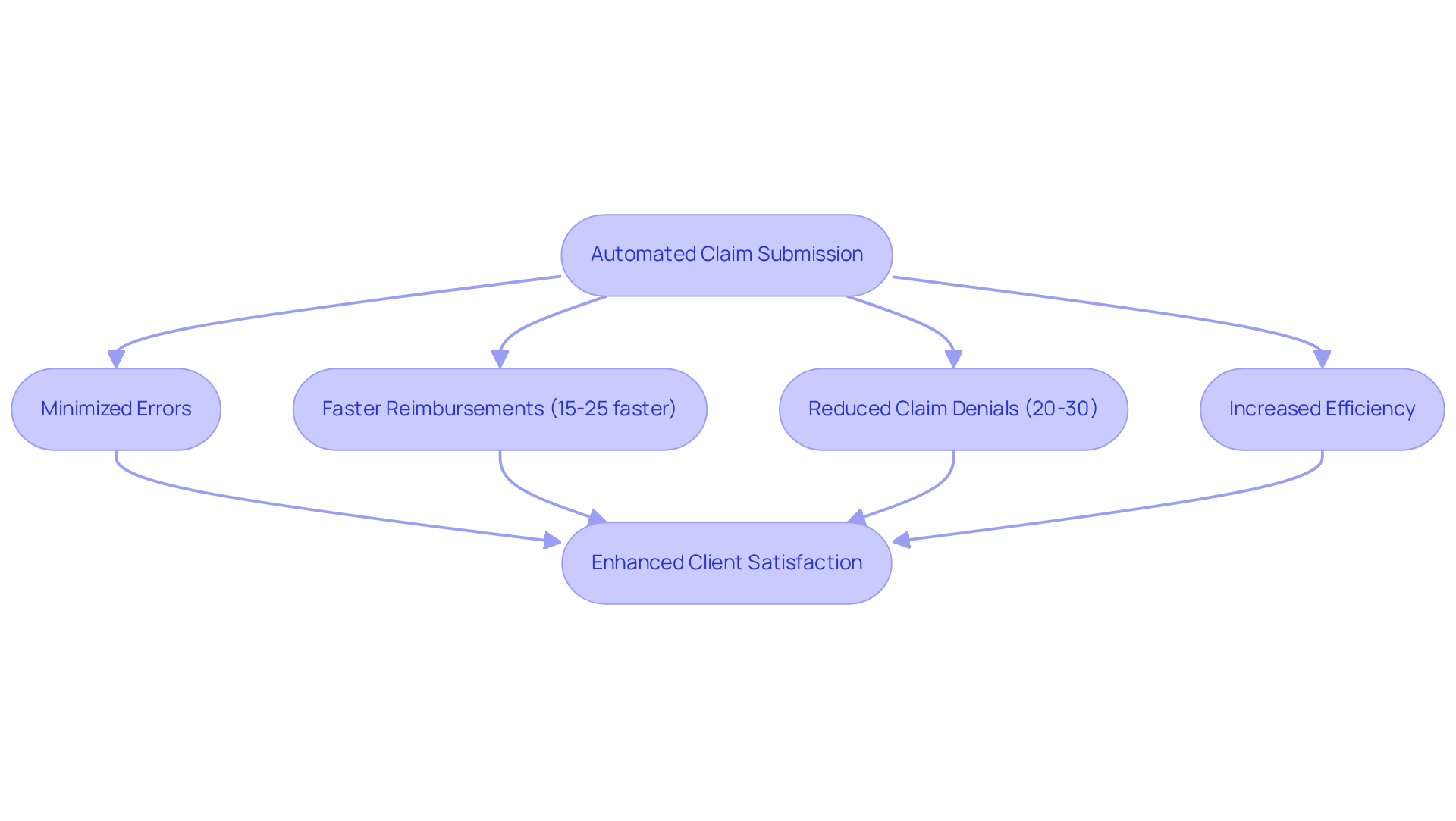
Real-Time Eligibility Verification allows healthcare providers to confirm an individual's insurance coverage and benefits instantly at the point of service. This capability is essential for ensuring that individuals qualify for the billed services, significantly reducing the risk of claim denials due to eligibility issues. By implementing this feature, practices can streamline their invoicing processes and enhance client satisfaction, leading to a 20-30% decrease in claim denials and faster reimbursement timelines. This proactive approach not only mitigates payment complications but also fosters trust and transparency, enabling patients to understand their costs upfront and avoid unexpected charges. Furthermore, integrating denial management strategies optimizes revenue cycle management, making it imperative for medical providers to adopt this technology to improve operational efficiency.
Comprehensive Reporting and Analytics
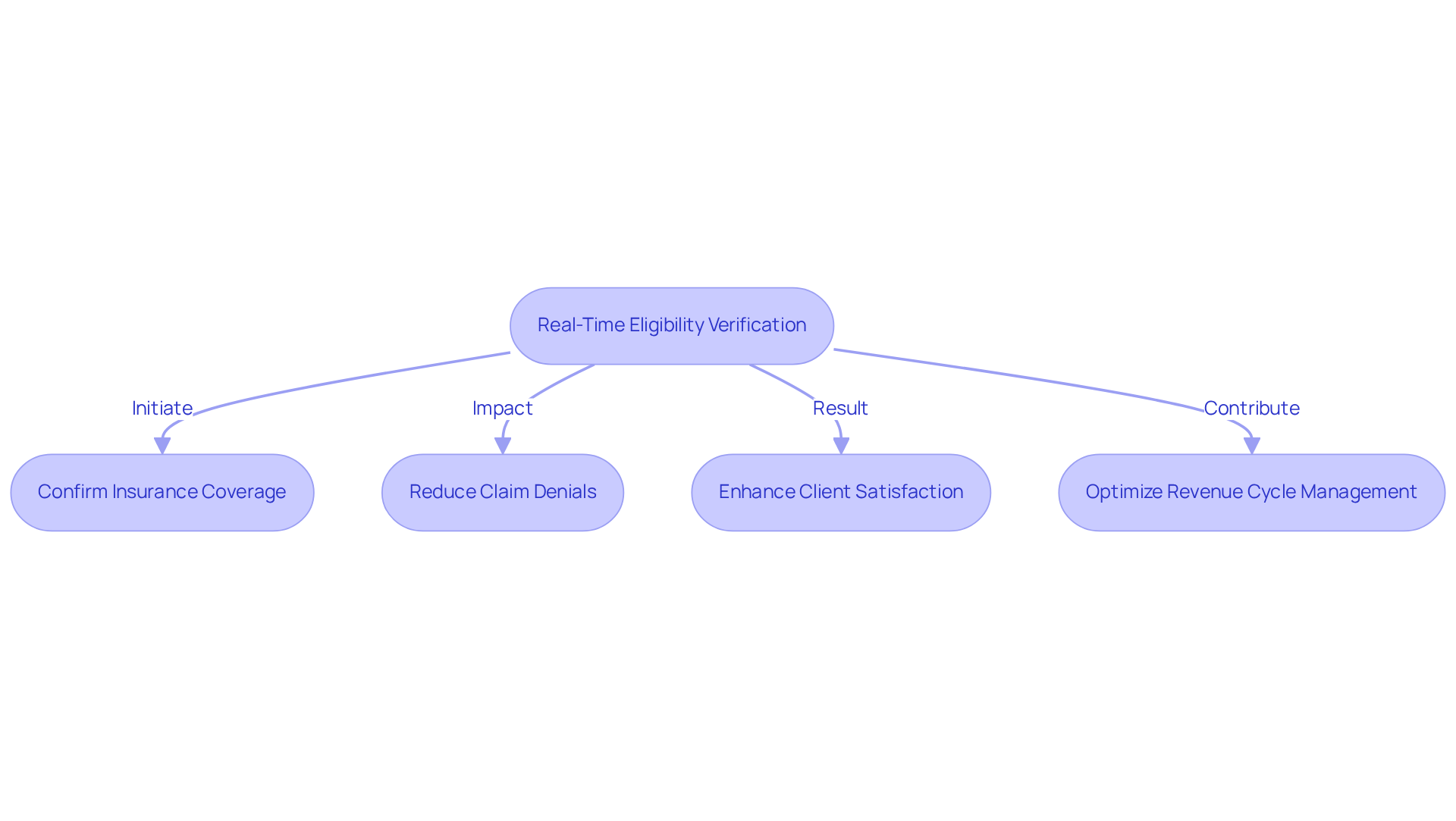
Comprehensive reporting and analytics tools empower healthcare providers to generate detailed reports on payment performance, claim statuses, and revenue trends. These insights are essential for identifying patterns, such as frequent claim denials or payment delays, which enable organizations to implement corrective measures effectively.
As we approach 2026, the integration of analytics in revenue cycle management is increasingly recognized as vital. Predictive analytics plays a significant role in forecasting trends and optimizing billing processes. By leveraging these tools, organizations can enhance their financial health, reduce claim denials - which can reach as high as 30% on first submission - and improve overall operational efficiency.
Key metrics to monitor include:
- Claim denial rates
- Days in receivables outstanding
- Clean claim rates
These metrics are crucial for maintaining a profitable practice. As the healthcare landscape evolves, utilizing analytics will be indispensable in managing the complexities of medical invoicing and ensuring sustainable revenue growth.
User-Friendly Interface
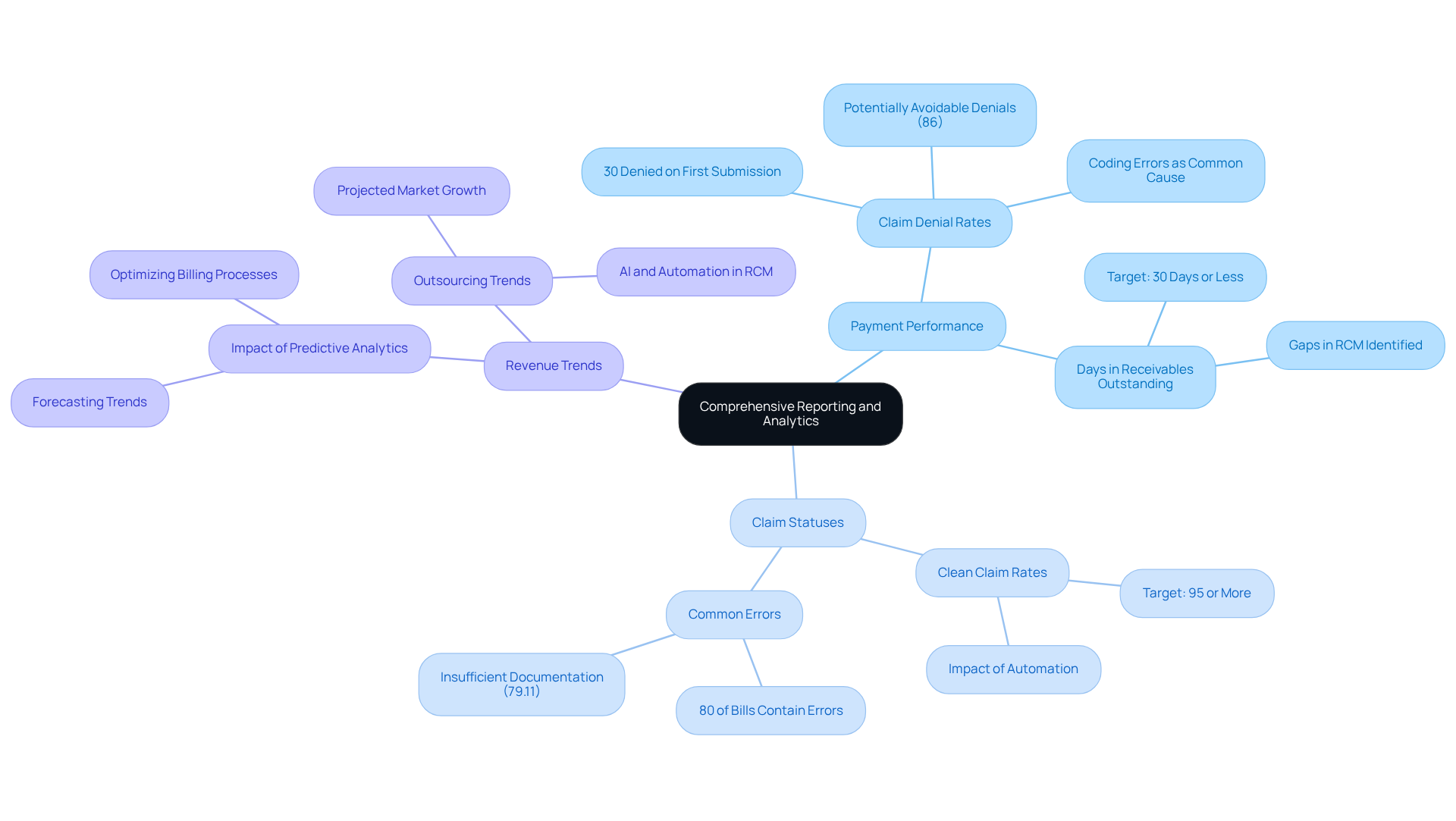
A user-friendly interface in medical invoicing software is crucial for simplifying navigation and reducing the learning curve for new users. Intuitive dashboards, easy access to key functions, and clear instructions empower staff to perform their tasks more efficiently. This usability is vital for minimizing errors and ensuring that payment processes operate smoothly.
Healthcare experts recognize that an intuitive design not only enhances operational efficiency but also significantly reduces the likelihood of invoicing errors, which can lead to financial losses and client dissatisfaction. By prioritizing user-friendly interfaces, practices can streamline their invoicing operations, ultimately improving cash flow and enhancing overall care for individuals.
EHR Integration
EHR integration facilitates a seamless connection between medical invoicing software and electronic health records, enabling the automatic transfer of client data. This integration markedly enhances invoicing accuracy by ensuring that invoicing information remains consistently precise and up-to-date, thereby minimizing errors typically associated with manual data entry. By streamlining these processes, medical practices can significantly improve their invoicing efficiency and, in turn, elevate the overall quality of care provided to patients.
Healthcare Partners Consulting's solutions have demonstrated:
- A 20-30% reduction in claim denials
- A 15-25% acceleration in reimbursement timelines
This underscores their effectiveness in optimizing revenue cycle management. Moreover, medical service providers have noted that automating invoicing tasks through EHR integration allows them to focus more on patient care rather than administrative duties. This shift ultimately leads to improved outcomes and greater patient satisfaction. As one provider articulated, 'EHR integration has transformed our invoicing process, enabling us to reduce errors and concentrate on what truly matters-our patients.
Customizable Billing Options
Customizable payment options empower healthcare providers to tailor their invoicing procedures to meet the specific needs of their operations. This flexibility includes:
- Establishing various payment plans
- Modifying invoicing cycles
- Creating personalized invoices
By implementing such adaptable payment strategies, organizations can significantly enhance client satisfaction. For instance, Healthcare Partners Consulting's comprehensive medical invoicing solutions have led to a 20-30% reduction in claim rejections and a 15-25% acceleration in reimbursement timelines.
Accommodating diverse financial circumstances through flexible payment options not only fosters trust but also encourages timely payments, ultimately enhancing overall revenue cycle management. Research indicates that organizations prioritizing adaptable payment choices experience increased client loyalty and satisfaction, as these options alleviate financial stress and contribute to a more positive experience for individuals. Moreover, tailored financial communications can improve the likelihood of clients settling their accounts on time by 20%.
By embracing personalized invoicing options, which include denial management and performance reporting, healthcare providers can cultivate a more supportive environment for their clients. This approach leads to improved retention rates and overall success in service delivery. To effectively implement these adaptable payment choices, organizations should regularly evaluate their invoicing procedures and solicit feedback from clients to ensure their needs are adequately addressed.
Robust Security Features
Strong security features in medical billing electronic claims software are essential for protecting sensitive individual information. These features encompass:
- Encryption
- Access controls
- Regular security audits
All critical for ensuring compliance with HIPAA regulations. By implementing these security measures, medical practices can significantly mitigate the risk of data breaches, which have become increasingly common in recent years. For example, a ransomware attack in 2024 compromised health records of over 190 million Americans, highlighting the urgent need for stringent security protocols.
Prioritizing security not only protects financial and reputational interests but also fosters trust with clients. When individuals are confident that their information is secure, they are more likely to engage with medical practitioners and share sensitive details. As cybersecurity specialist Wenda Hendren notes, "HIPAA compliance in medical billing also warrants significant focus," underscoring the importance of effective data protection in maintaining patient trust and ensuring the long-term success of medical practices. In the current landscape, where 23% of business leaders identify hybrid work as their primary breach threat, robust security measures are not merely a regulatory obligation but a fundamental aspect of ethical service delivery.
Denial Management Tools
Denial management tools are crucial for healthcare providers, allowing them to effectively track, analyze, and resolve claim denials. These tools provide valuable insights into the underlying reasons for denials, which may include inaccuracies in patient data or insufficient documentation. By streamlining the appeals process, organizations can recover lost revenue and bolster their financial stability.
Implementing robust denial management strategies, such as those offered by Healthcare Partners Consulting, not only enhances cash flow but also significantly reduces the administrative workload associated with claim rework. Organizations that prioritize denial management have reported a 20-30% reduction in claim denials, alongside improved cash flow, with effective strategies leading to faster reimbursement timelines.
Key features of these tools include:
- Intake support, encompassing consents and demographic capture.
- Monthly performance reporting with KPI tracking.
As healthcare administrators emphasize, focusing on accurate documentation and proactive eligibility verification is essential for minimizing denials and ensuring timely reimbursements. By leveraging medical billing electronic claims software, clinics can transform their revenue cycle management, ultimately paving the way for a more sustainable financial future.
Customer Support and Training
Effective customer support and training services are essential for healthcare providers aiming to maximize the utilization of their financial software. These resources typically encompass:
- Access to help desks
- Comprehensive training sessions
- Detailed user manuals
Investing in thorough training can significantly enhance invoicing efficiency, equipping staff to navigate the software proficiently. This not only optimizes the software's capabilities but also minimizes disruptions in payment processes, which in turn leads to improved cash flow and operational stability.
As observed by medical providers, well-trained accounting personnel are crucial for ensuring accuracy and compliance. This ultimately contributes to the financial health of the organization.
Healthcare Partners Consulting: Tailored Administrative Support
Healthcare Partners Consulting (HPC) provides specialized administrative assistance tailored to the distinct needs of medical and mental health facilities. Their comprehensive invoicing solutions and operational management consulting empower medical providers to concentrate on delivering exceptional care, while HPC adeptly manages the complexities of invoicing and administrative tasks, including medical billing electronic claims software, scheduling, and document handling. This collaboration not only alleviates the administrative burden but also boosts operational efficiency, enabling clinics to excel in a competitive landscape.
By capitalizing on HPC's expertise, mental health clinics can optimize their operations, leading to enhanced revenue cycles and decreased overhead costs. The impact of customized administrative support is significant; organizations report a heightened focus on client interactions and care quality. Testimonials from healthcare providers underscore the advantages of partnering with consulting firms like HPC, highlighting improvements in billing accuracy and overall operational management. This strategic alliance ultimately fosters better outcomes for individuals and promotes a more sustainable operational model.
With HPC's bespoke administrative support, providers can prioritize what truly matters - caring for their patients. To discover how HPC can help optimize your practice, visit our Consulting page today.
Conclusion
The advantages of medical billing electronic claims software are evident, underscoring its critical role in enhancing the efficiency and effectiveness of healthcare billing practices. By automating claim submissions, verifying eligibility in real-time, and integrating comprehensive reporting tools, providers can significantly reduce errors, improve cash flow, and ultimately concentrate more on patient care. The software's user-friendly interface and robust security features further ensure that practices can operate smoothly while safeguarding sensitive information.
Key insights from the article reveal that features such as denial management tools and customizable billing options can lead to a significant reduction in claim denials and an increase in patient satisfaction. The emphasis on customer support and training highlights the necessity of fully utilizing these systems to maximize their benefits. As healthcare continues to evolve, the integration of these essential features will be crucial for practices aiming to excel in a competitive environment.
Embracing medical billing electronic claims software transcends mere technological adoption; it represents a transformation in how healthcare providers manage their operations. By prioritizing these features, organizations can enhance their revenue cycles, bolster patient trust, and ultimately deliver higher quality care. For those seeking to optimize their billing processes, investing in the appropriate software and support systems is a vital step toward achieving a more efficient and patient-centered practice.
Frequently Asked Questions
What is automated claim submission in medical billing?
Automated claim submission allows healthcare providers to electronically submit claims to insurance payers without manual intervention, minimizing errors and expediting the claims process.
How does automated claim submission benefit healthcare practices?
It results in reimbursements that are typically 15-25% faster, reduces claim denials by 20-30%, and alleviates administrative burdens, allowing staff to focus on client interactions and care.
What additional features does automated claim submission include?
The process includes denial management and appeals, ensuring that underpaid or denied claims are addressed effectively.
What is real-time eligibility verification?
Real-time eligibility verification allows healthcare providers to instantly confirm an individual's insurance coverage and benefits at the point of service.
How does real-time eligibility verification impact claim denials?
It significantly reduces the risk of claim denials due to eligibility issues, leading to a 20-30% decrease in claim denials and faster reimbursement timelines.
What advantages does real-time eligibility verification provide to patients?
It fosters trust and transparency by enabling patients to understand their costs upfront and avoid unexpected charges.
What are comprehensive reporting and analytics tools in medical billing?
These tools allow healthcare providers to generate detailed reports on payment performance, claim statuses, and revenue trends, helping to identify patterns and implement corrective measures.
Why is predictive analytics important for healthcare providers?
Predictive analytics helps in forecasting trends and optimizing billing processes, which is vital for enhancing financial health and reducing claim denials.
What key metrics should healthcare providers monitor for effective revenue cycle management?
Key metrics include claim denial rates, days in receivables outstanding, and clean claim rates, which are crucial for maintaining a profitable practice.

