
What Does Revenue Cycle Mean in Healthcare for Mental Health Clinics?
Introduction
Understanding the complexities of revenue cycle management (RCM) is essential for mental health clinics aiming for financial stability and operational efficiency. This comprehensive process, which encompasses patient registration through to final payment, presents unique challenges in the field of psychological services. The diversity of insurance policies and varying reimbursement rates complicates this landscape. As clinics navigate these financial intricacies, a critical question emerges: how can they optimize their RCM strategies to enhance cash flow while ensuring high-quality patient care in the face of increasing operational demands?
Define Revenue Cycle Management in Healthcare
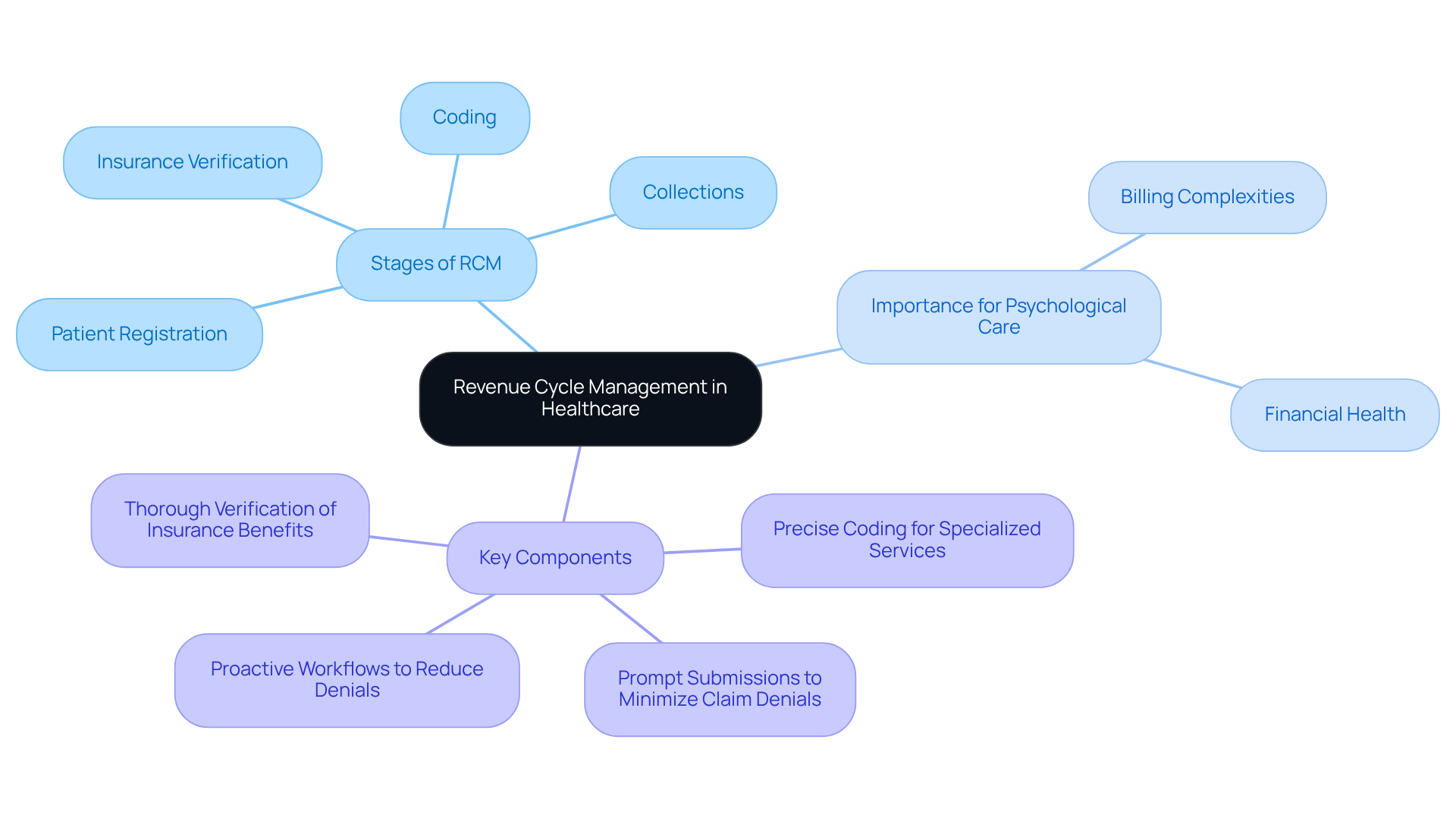
To understand what does revenue cycle mean in healthcare, it refers to the entire financial process that providers utilize to manage revenue from the initial appointment to the final payment. This process includes crucial stages such as patient registration, insurance verification, coding, and collections. For psychological care facilities, effective RCM is essential due to the unique billing complexities associated with psychological services, which often involve diverse insurance policies and varying reimbursement rates.
Healthcare Partners Consulting brings over 37 years of expertise in enhancing RCM, ensuring quicker payments, fewer write-offs, and improved cash flow-elements that are vital for sustaining the financial health of your practice. Statistics indicate that practices implementing robust RCM strategies can experience a 20-30% improvement in cash flow within the first year, highlighting the financial advantages of streamlined operations.
Key components of effective RCM in clinics focused on psychological care include:
- Precise coding for specialized services
- Prompt submissions to minimize claim denials
- Thorough verification of insurance benefits to prevent unexpected denials
Furthermore, our proactive workflows reduce denials, streamline documentation, and identify issues before they affect reimbursement.
Effective RCM establishes a stable financial foundation, enabling you to deliver high-quality care, invest in staff, and expand your services to meet the needs of patients in your community. Additionally, psychological care facilities must navigate challenges such as telehealth invoicing and varying payer regulations, which further complicate the RCM process.
Insights from industry specialists, including Davia Ward, emphasize the ongoing billing crisis related to well-being, underscoring the necessity for comprehensive strategies to enhance financial stability. By addressing these components-such as transparent reporting and regular audits-clinics focused on psychological well-being can improve their financial sustainability and concentrate more on delivering quality care.
Outline the Stages of the Revenue Cycle Process
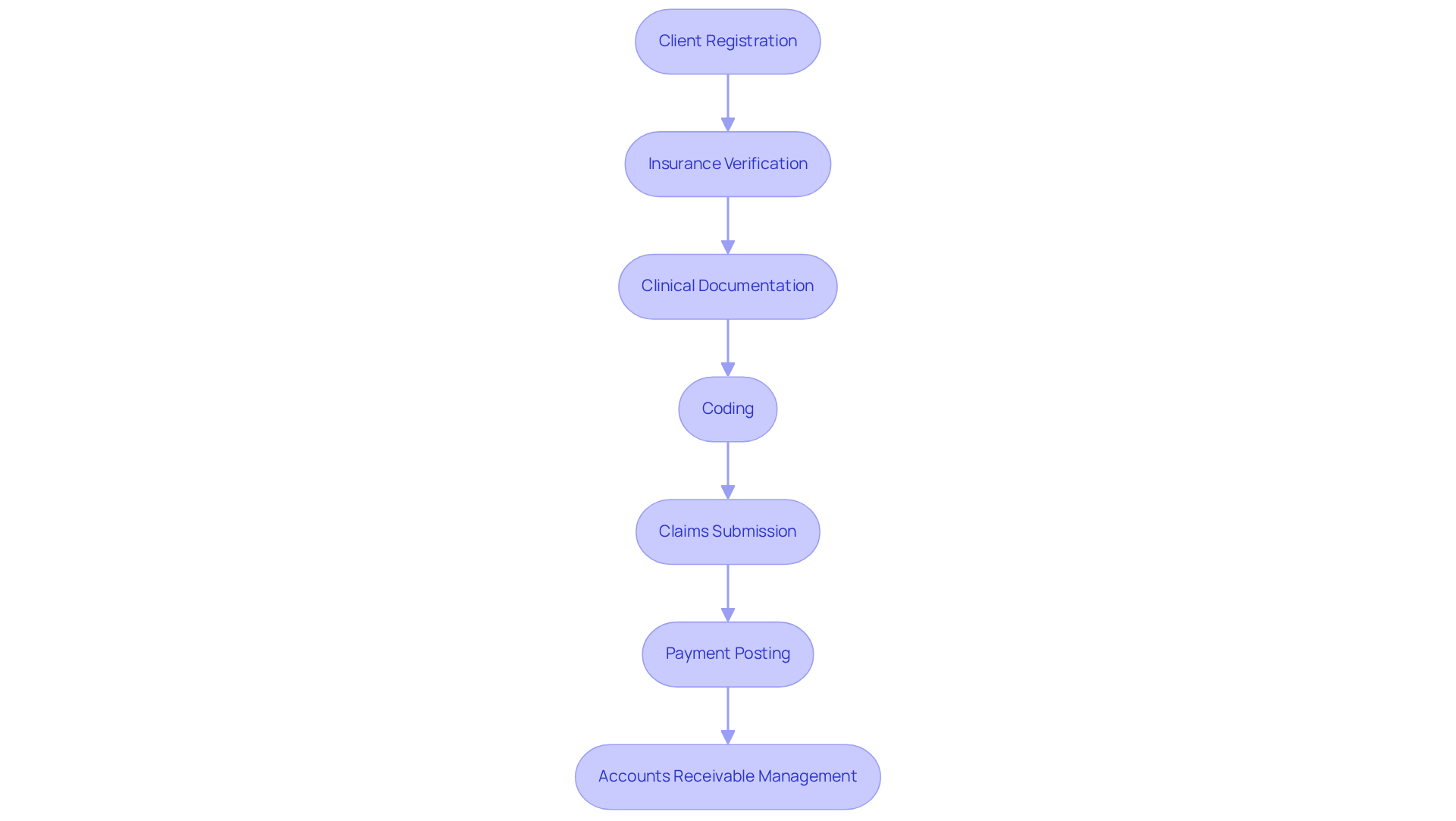
The revenue cycle process encompasses several critical stages essential for the financial health of mental health clinics:
- Client Registration: This initial stage involves gathering extensive individual information and insurance details at the time of scheduling. Accurate data capture is vital to prevent downstream issues, such as claim denials due to incorrect information.
- Insurance Verification: Prior to the appointment, confirming the individual's insurance coverage and benefits is crucial. This step helps set clear financial expectations and reduces the risk of collection issues. For instance, a specialty clinic may confirm benefits two days before appointments, notifying individuals of any increased out-of-pocket contributions necessary by their insurance plans.
- Clinical Documentation: Thorough documentation of the patient's treatment and services provided is essential. Precise clinical records assist in payment processes and compliance, ensuring that all services rendered are recorded and charged correctly.
- Coding: This stage involves assigning the correct codes for diagnoses and procedures, which is essential for enabling precise invoicing. Proper coding helps avoid claim denials and ensures compliance with payer requirements. Expert mental and behavioral health invoicing services, such as those offered by Healthcare Partners Consulting, enhance revenue cycle management through accurate coding and compliance.
- Claims Submission: After coding, claims are sent to insurance companies for reimbursement. Effective claim submission processes, including claim scrubbing, ensure that claims are clean and compliant, leading to faster payments.
- Payment Posting: This stage records payments received from both insurance and patients. Accurate payment posting is vital for maintaining financial visibility and ensuring that accounts receivable data remains precise.
- Accounts Receivable Management: Monitoring outstanding balances and following up on unpaid claims is crucial for optimizing cash flow. Efficient accounts receivable management, as supported by Healthcare Partners Consulting, assists clinics in recovering revenue lost due to invoicing errors or insurance disputes. Their proactive follow-up on unpaid claims and appeal submissions can lead to a 20-40% reduction in accounts receivable days and noticeable improvements in monthly collections and cash flow.
Each of these stages plays a significant role in ensuring that clinics focused on wellness grasp what does revenue cycle mean in healthcare to maximize revenue while minimizing delays in payment, ultimately supporting their operational sustainability. Insights from industry specialists such as Davia Ward also underscore the ongoing difficulties in psychological care invoicing, stressing the necessity for effective solutions to tackle these concerns.
Explain the Importance of Revenue Cycle Management
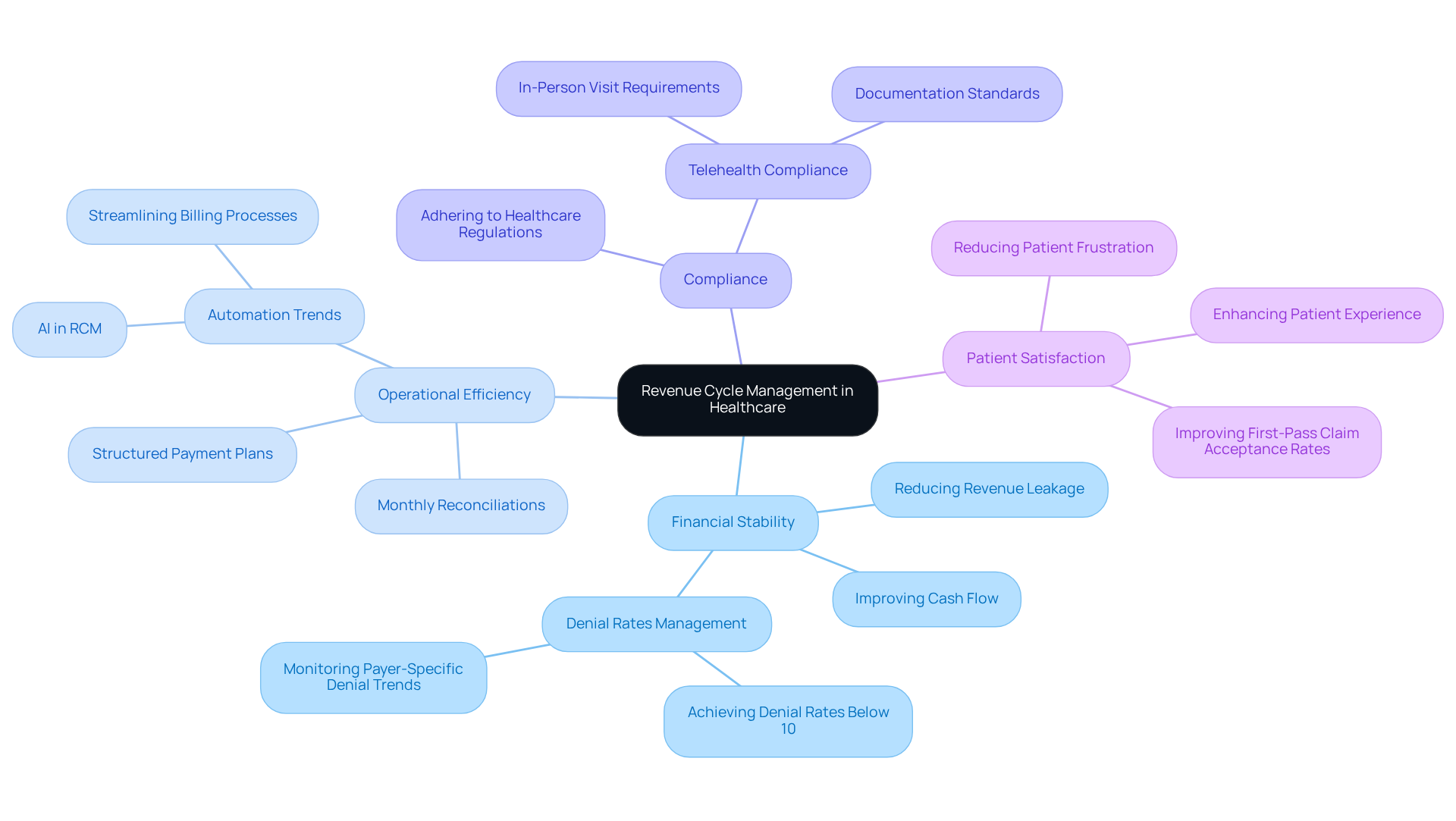
For healthcare providers, especially mental health clinics, understanding what revenue cycle means in healthcare is crucial as it plays a significant role in their financial stability and operational efficiency. Effective RCM highlights what revenue cycle means in healthcare by allowing clinics to capture all revenue owed for services rendered, thereby reducing revenue leakage that can arise from billing errors or claim denials. For example, organizations that adopt robust RCM practices often achieve denial rates between 8% and 10%, with collection rates surpassing 97%. This not only enhances cash flow but also enables clinics to reinvest in improved care for individuals and operational enhancements.
Moreover, understanding what revenue cycle means in healthcare is essential for ensuring compliance with stringent healthcare regulations, which is vital in the highly regulated psychological services sector. By optimizing invoicing procedures, RCM fosters clarity and efficiency, ultimately improving the experience for individuals receiving care. Key services, such as coordinating structured payment plans and conducting monthly reconciliations, further bolster cash flow and operational effectiveness. As healthcare leaders increasingly recognize the link between patient satisfaction and financial performance, investing in effective RCM practices emerges as a strategic priority for clinics aiming to thrive in a competitive landscape. Insights from Davia Ward highlight the persistent challenges in mental wellness invoicing, underscoring the necessity for robust RCM solutions to guarantee continuous, high-quality care. Additionally, with 75% of healthcare finance leaders identifying automation as a top initiative for 2026, the trend towards investing in RCM practices is unmistakable.
Identify Challenges in Revenue Cycle Management
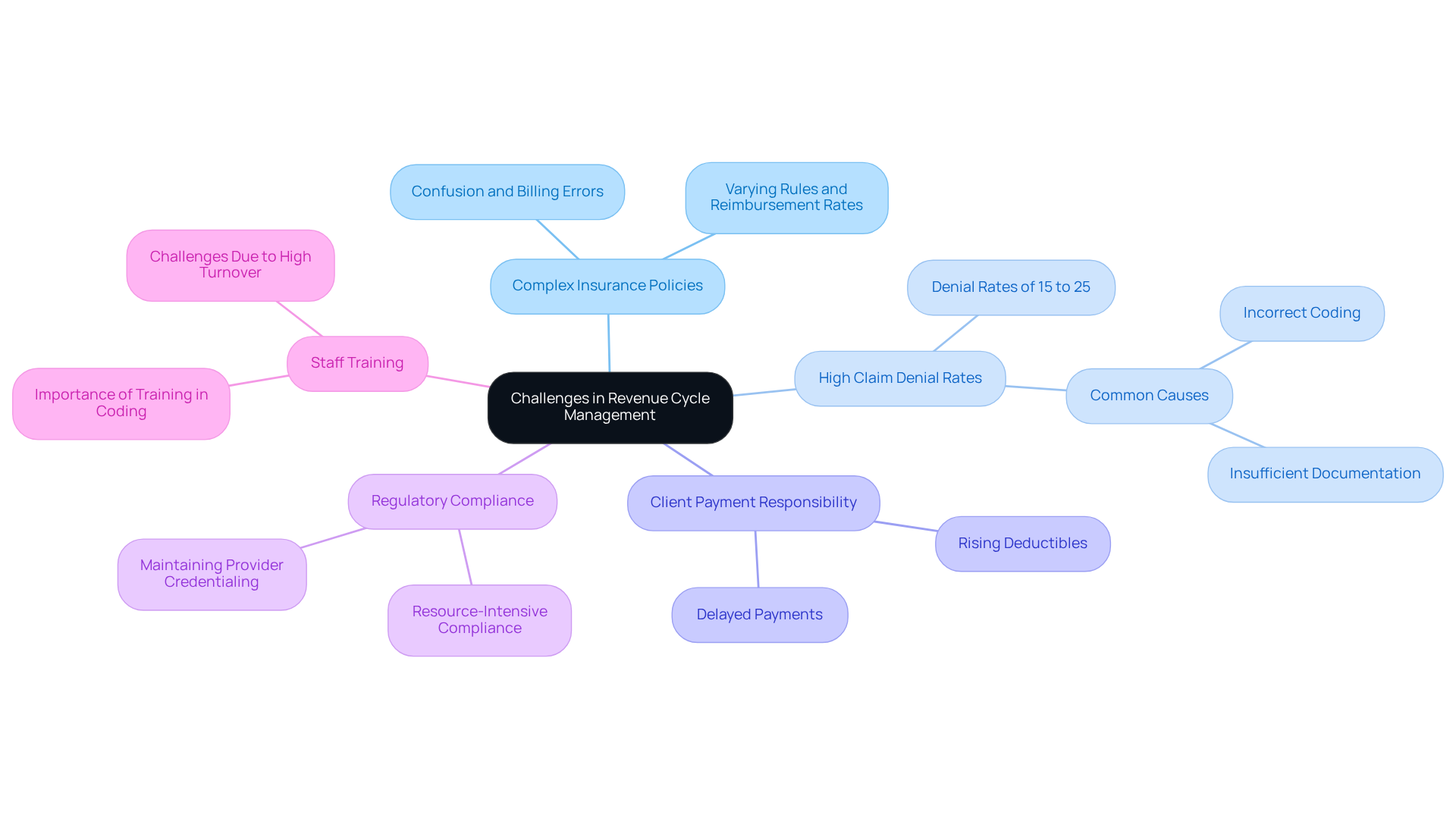
Mental wellness clinics encounter significant challenges in Revenue Cycle Management, which can hinder their financial sustainability and operational efficiency. The primary issues include:
- Complex Insurance Policies: The insurance landscape is intricate, characterized by varying rules and reimbursement rates across providers. This complexity often results in confusion and billing errors, adversely affecting revenue.
- High Claim Denial Rates: Mental wellness services are particularly susceptible to claim denials, with rates ranging from 15% to 25%, markedly higher than the 5-10% seen in other medical specialties. Common causes of these denials include incorrect coding and insufficient documentation, which can lead to rejections. Incomplete therapy notes that do not adequately describe client symptoms and treatment goals are critical factors contributing to these denials. Healthcare Partners Consulting specializes in mental and behavioral health coding, ensuring that every claim submitted accurately reflects the services provided and complies with payer-specific guidelines, thereby reducing the risk of denials. Our team is well-versed in the nuances of coding, including the appropriate application of modifiers, to further minimize errors.
- Client Payment Responsibility: As deductibles rise, individuals are increasingly responsible for larger portions of their bills. This shift complicates collections and can result in delayed payments, further straining clinic finances.
- Regulatory Compliance: Compliance with healthcare regulations is essential but can be resource-intensive. Clinics must navigate complex requirements, including maintaining updated provider credentialing records to avoid claim denials related to eligibility issues. This focus on compliance can detract from patient care and operational efficiency. HPC's comprehensive denial management services address these compliance challenges by managing coding, timely filing, prior authorization, and medical necessity denials.
- Staff Training: Ensuring that staff are adequately trained in invoicing and coding practices is crucial for minimizing errors and maximizing revenue. However, high turnover rates and limited resources can complicate consistent training efforts. HPC offers tailored coding support and training to enhance staff capabilities, ensuring accurate coding and improved billing outcomes.
Addressing these challenges is vital for optimizing what does revenue cycle mean in healthcare, while also enhancing cash flow and securing the financial health of therapy clinics. Implementing real-time insurance eligibility verification can help identify coverage issues early, while standardizing documentation and authorization workflows can improve outcomes and reduce claim denials. Through proficient programming and proactive denial management strategies, Healthcare Partners Consulting can significantly enhance revenue cycle efficiency for psychological practices.
Suggest Strategies for Optimizing Revenue Cycle Management
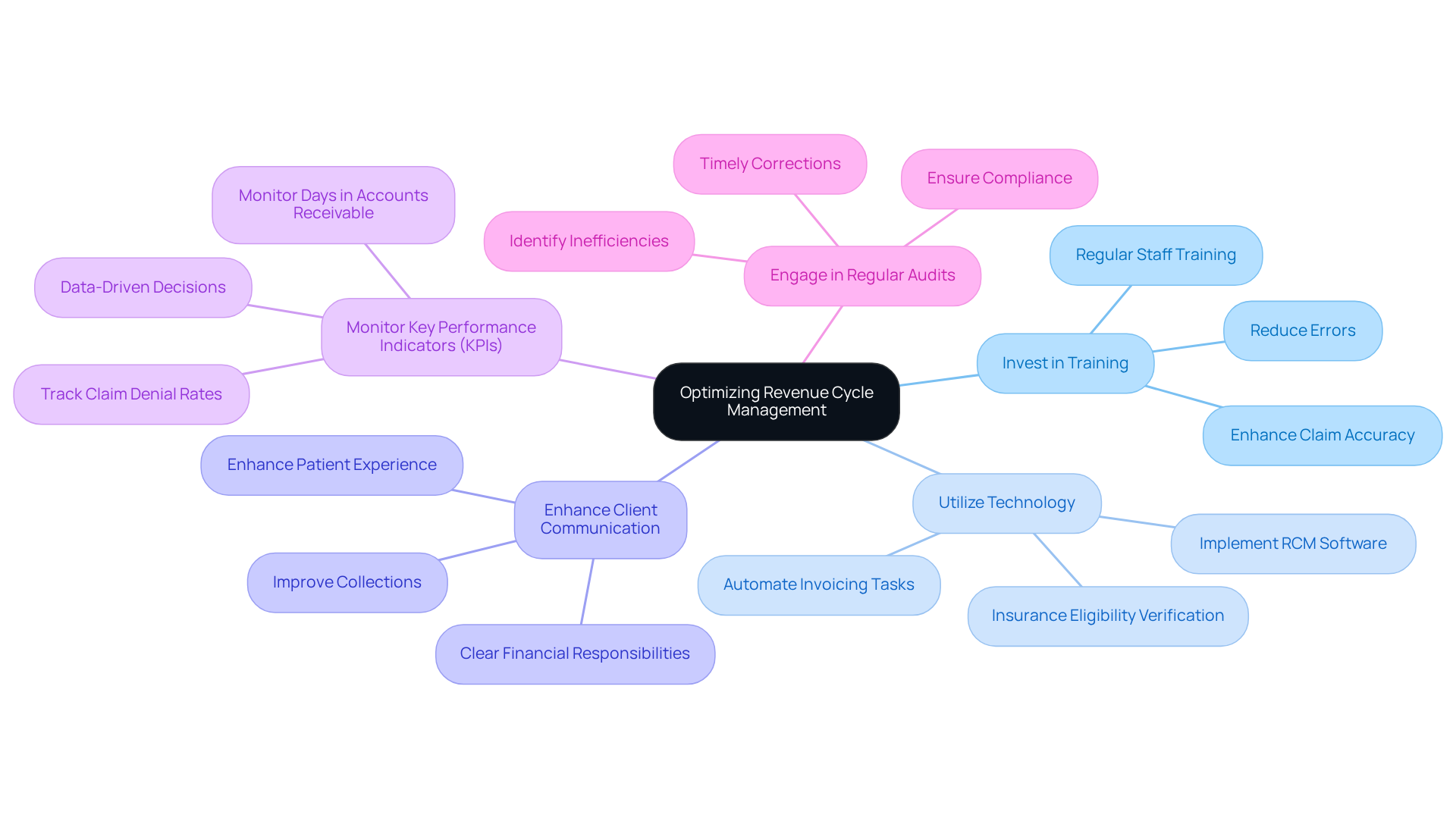
To effectively optimize Revenue Cycle Management (RCM) in mental health clinics, consider implementing the following strategies:
- Invest in Training: Regular training for staff on invoicing and coding practices is essential. This investment can significantly reduce errors and enhance the accuracy of claim submissions, ultimately leading to improved reimbursement rates.
- Utilize Technology: Implementing RCM software can streamline processes, automate invoicing tasks, and enhance data accuracy. For instance, automated insurance eligibility verification can greatly decrease billing workflow time, enabling staff to concentrate on care.
- Enhance Client Communication: Clear communication with clients regarding their financial responsibilities is crucial. This practice improves collections, reduces confusion, and enhances the overall patient experience.
- Monitor Key Performance Indicators (KPIs): Regularly tracking KPIs such as claim denial rates and days in accounts receivable is vital for identifying areas needing improvement. This data-driven approach allows clinics to make informed decisions that enhance financial performance. Clients of Healthcare Partners Consulting typically see a 20-40% reduction in days in accounts receivable, significantly improving cash flow.
- Engage in Regular Audits: Conducting audits of invoicing practices can reveal inefficiencies and ensure adherence to healthcare regulations. Regular reviews help identify gaps in the revenue cycle, allowing for timely corrections and optimizations. Insights from Davia Ward highlight the ongoing psychological billing crisis, emphasizing the need for accurate coding and compliance to effectively address these challenges.
By adopting these strategies, mental health clinics can enhance their revenue cycle processes, which raises the question of what does revenue cycle mean in healthcare, leading to improved financial outcomes and better patient care.
Conclusion
Understanding the complexities of revenue cycle management (RCM) is essential for mental health clinics, as it directly influences their financial stability and operational effectiveness. By adeptly managing the revenue cycle-from patient registration to final payment-clinics can optimize revenue capture, reduce denials, and ultimately improve the quality of care provided to their clients.
This article outlines the critical stages of the revenue cycle process, highlighting the necessity of accurate coding, timely claim submissions, and comprehensive insurance verification. It also examines the specific challenges encountered by mental health providers, such as elevated claim denial rates and intricate insurance policies, which can substantially impact cash flow and operational efficiency. Implementing strategies to address these challenges, including staff training, technology integration, and regular audits, is crucial for establishing a robust RCM framework.
In conclusion, prioritizing effective revenue cycle management not only bolsters the financial health of mental health clinics but also ensures their capacity to deliver high-quality services to those in need. By investing in RCM practices and proactively addressing challenges, clinics can enhance their operational sustainability, ultimately benefiting both their organization and the communities they serve. Adopting these strategies will lead to improved financial outcomes and a more favorable patient experience.
Frequently Asked Questions
What is revenue cycle management (RCM) in healthcare?
Revenue cycle management in healthcare refers to the entire financial process that providers use to manage revenue, starting from the initial appointment to the final payment. It includes stages like patient registration, insurance verification, coding, and collections.
Why is effective RCM important for psychological care facilities?
Effective RCM is crucial for psychological care facilities due to the unique billing complexities associated with psychological services, which involve diverse insurance policies and varying reimbursement rates.
What are the key components of effective RCM in psychological care clinics?
Key components include precise coding for specialized services, prompt submissions to minimize claim denials, and thorough verification of insurance benefits to prevent unexpected denials.
How can implementing robust RCM strategies impact cash flow?
Practices that implement robust RCM strategies can experience a 20-30% improvement in cash flow within the first year, contributing to the financial health of the practice.
What stages are involved in the revenue cycle process?
The stages involved in the revenue cycle process include: 1. Client Registration 2. Insurance Verification 3. Clinical Documentation 4. Coding 5. Claims Submission 6. Payment Posting 7. Accounts Receivable Management
What is the significance of accurate client registration?
Accurate client registration is vital to prevent downstream issues, such as claim denials due to incorrect information. It involves gathering extensive individual and insurance details at the time of scheduling.
How does insurance verification contribute to the revenue cycle?
Insurance verification helps set clear financial expectations and reduces the risk of collection issues by confirming an individual's insurance coverage and benefits before the appointment.
Why is clinical documentation important in the revenue cycle?
Thorough clinical documentation ensures that all services rendered are recorded and charged correctly, which is essential for payment processes and compliance.
What role does coding play in revenue cycle management?
Coding involves assigning the correct codes for diagnoses and procedures, which is essential for accurate invoicing and helps avoid claim denials while ensuring compliance with payer requirements.
How does payment posting affect financial visibility?
Payment posting records payments received from both insurance and patients, which is vital for maintaining financial visibility and ensuring that accounts receivable data remains precise.
What is accounts receivable management and its importance?
Accounts receivable management involves monitoring outstanding balances and following up on unpaid claims. Efficient management is crucial for optimizing cash flow and recovering revenue lost due to invoicing errors or insurance disputes.
What challenges do psychological care facilities face in RCM?
Psychological care facilities face challenges such as telehealth invoicing and varying payer regulations, which complicate the RCM process.

