Wound Care for Elderly Thin Skin: Best Practices and Treatments
Wound Care for Elderly Thin Skin: Best Practices and Treatments
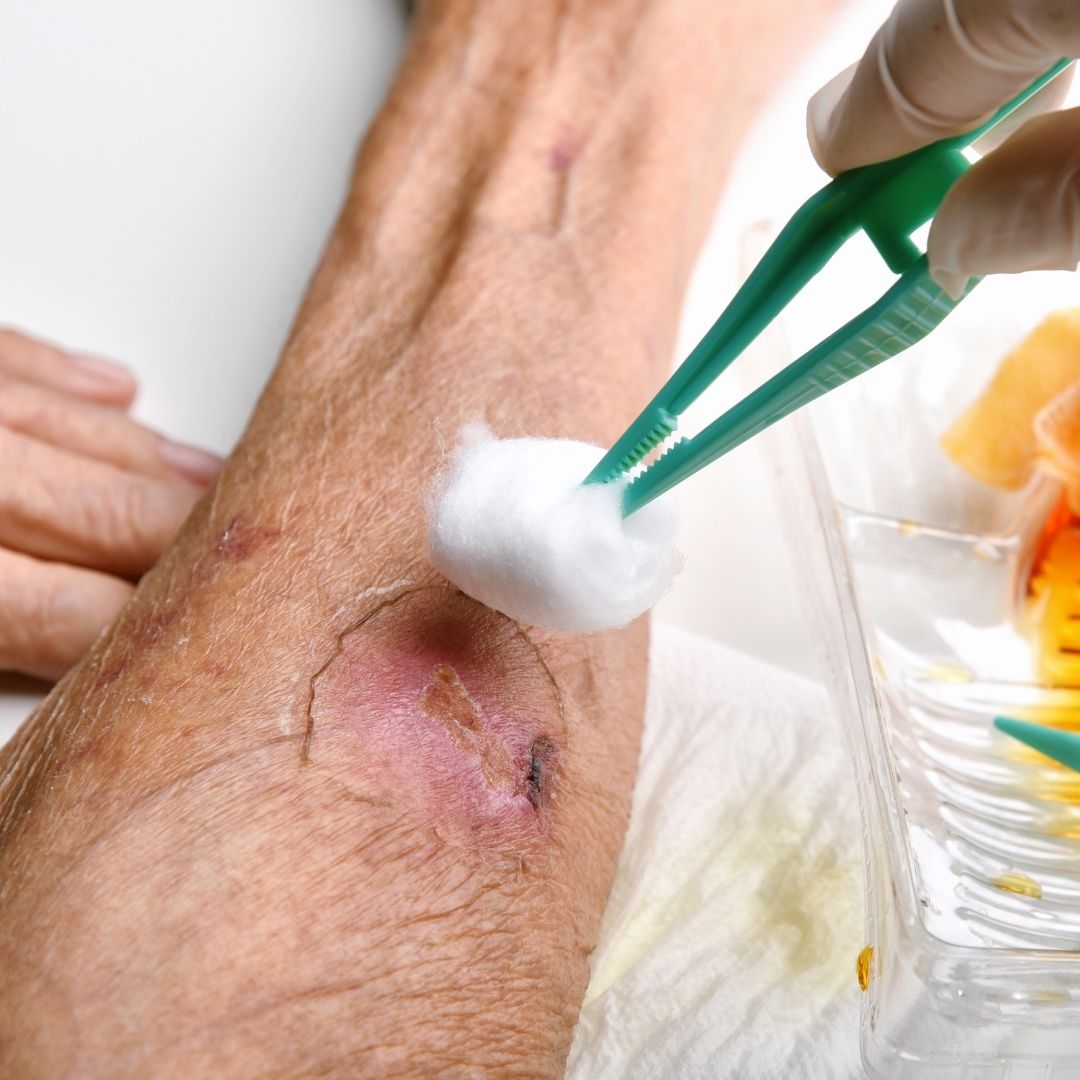
Wound care for elderly skin and older adults requires a thoughtful, proactive approach. As we age, our skin becomes thin and fragile due to reduced collagen and general lifestyle factors. Because of this, even routine care, such as removing gauze stuck to wounds, can result in skin tears and infections.
Additionally, improper wound care can significantly increase the risk of complications. This includes infection risk, chronic and non-healing wounds, skin tears, and systemic complications. Unlike younger skin, thin elderly skin requires specialized wound care strategies that prioritize gentle cleansing, wound protection, and continuous monitoring.
At Royal Wound Care, proper education is the cornerstone of accessible, compassionate care. That’s why today, we’re sharing a patient-focused guide on wound care for elderly skin. We will discuss evidence-based strategies that support optimal healing, reduce the risk of infection, and improve patient outcomes. Healing doesn’t have to be complex—you just need the right team to guide you through recovery.

Wound Care for Elderly Thin Skin: Best Practices and Treatments
There are many differences between young and elderly skin—especially in wound care. For example, fragile skin is much more susceptible to skin tears, pressure injuries, adhesive-related injuries (MARSI), and delayed healing. Over time, the natural aging process results in a loss of cushioning, structure, sweat and oil protection, and subcutaneous fat. This happens regardless of lifelong skincare habits.
As a result, minor wounds that may heal more quickly in younger adults can escalate rapidly in elderly patients. However, while these vulnerabilities matter, they should not result in delayed treatment or assumptions that slow healing is unavoidable. Instead, they highlight the importance of proper care techniques—many of which we are discussing today.
We will discuss common causes of thin skin in elderly patients and how to successfully treat thin-skin wounds. Proper wound-healing techniques are the foundation for fewer complications and an overall improved quality of life.
Related: “How Long Does It Take for a Wound to Heal?”

What Causes Thin Skin in Elderly Individuals?
Natural Aging
As we age, many factors contribute to the process of natural aging. Collagen and cell turnover decrease, subcutaneous fat decreases, sweat and oil gland activity slows, and hormonal activity changes. This is entirely natural—the skin isn’t designed to remain as resilient as it once was.
However, this slows healing, increases vulnerability, and decreases the immune response. Skin becomes more prone to injuries from continuous pressure and minor friction, and a weakened immune system can’t heal wounds as efficiently.
Chronic Sun Exposure
Chronic sun exposure often causes photoaging, a process in which UV radiation damages the skin’s structure. Most commonly, people associate this damage with wrinkles, fine lines, and hyperpigmentation. However, for wound care, the effects are far more than skin deep.
Here is how chronic sun exposure results in skin thinning:
UVA rays break down collagen, also known as the natural scaffolding and structure of the skin. This results in significant thinning and sagging.
Chronic sun exposure reduces cellular turnover, the process responsible for accelerating healing, reducing risk of infection, and replacing damaged cells (re-epithelialization).
As UV rays degrade structural proteins, such as collagen and elastin, they simultaneously increase reactive oxygen species (ROS). Together, these factors reduce skin thickness and increase susceptibility to skin bruising and tearing.
Sunlight is beneficial for the immune system. However, prolonged exposure can impair immune defenses and weaken the skin’s protective barrier.
When spending time in the sun, it’s important to prioritize protective clothing, including long-sleeve shirts, wide-brimmed hats, and sunglasses. Additionally, ensure you’re applying broad-spectrum sunscreen with SPF 30–50+ every 2 hours.
Medications
Certain medications can contribute to skin thinning, especially those used long-term or at high doses. Examples of medications that can lead to skin thinning include:
Corticosteroids: Prednisone, hydrocortisone, dexamethasone, and budesonide to treat pain, swelling, and additional immune system dysfunction
Blood Thinners: Apixaban, Warfarin, Rivaroxaban, and aspirin to prevent blood clots from forming or growing
GLP-1 Weight Loss Medications: Ozempic, Wegovy, Mounjaro, and Zepbound, originally prescribed to manage type 2 diabetes but increasingly prescribed for weight management
Chemotherapy Medications: Alkylating agents, antimetabolites, plant alkaloids, and anti-tumor antibiotics to prevent or treat cancer cells
It’s important to continue following your clinician's treatment plan, as these medications may be necessary for general quality of life. However, many decrease collagen synthesis, increase skin thinning and fragility, and cause significant dryness.
If you are concerned about skin fragility, contact your physician about medication management—do not discontinue use without consultation.
Poor Circulation
Poor circulation restricts blood flow to certain areas, limiting the delivery of oxygen and nutrients the body needs for regeneration. Without proper blood flow, the affected areas then become inflamed and swollen, stretching and thinning the skin over time. This is commonly known as edema.
Additionally, the lack of oxygen and nutrients prevents the body from producing collagen effectively, leading to a loss of structural integrity. Sometimes, poor circulation results from smoking, blood clots, or long periods of sitting. Other times, however, pre-existing conditions such as varicose veins, Raynaud’s disease, and peripheral artery disease can result in poor circulation.
Related: Edema and Diabetes and Slow Healing Wounds: Understanding Care
Nutrition and Hydration
Our diets play a crucial role in skin health. Nutrient-dense foods, such as colorful vegetables, fatty fish, and whole grains, support collagen production and cellular regeneration. Poor nutrition, on the other hand, can result in glycation—a process that damages collagen and elastin, leading to skin thinning.
Alongside a nutrient-dense diet, proper hydration is essential for counteracting thin, fragile skin. In fact, research shows that high water consumption positively impacts skin physiology. Without adequate hydration, skin cells cannot receive the water necessary to maintain their structural integrity.
For additional information, we kindly encourage you to read: “What to Eat for Faster Wound Healing.”
Medical Conditions
As discussed previously, certain pre-existing conditions can directly result in significant skin thinning. Examples of medical conditions that contribute to skin thinning include:
Diabetes
Cushing’s syndrome
Scleroderma
Chronic Constructive Pulmonary Disease (COPD)
Chronic renal failure
Kidney disease
Ehlers-Danlos syndrome
Individuals with the above conditions are often considered high-risk patients, requiring advanced wound care planning and closer monitoring.
Most Common Injury for Elderly Thin Skin
Skin tears are among the most commonly treated wounds in older adults. In their most basic form, a skin tear is when the top layer of skin separates from the underlying tissue, resulting in uneven torn skin flaps. Typically, they result from shear, friction, and blunt force—such as falls, adhesive removal, or bumping into objects.
Additionally, in treatment, skin tears follow a unique classification system, allowing clinicians to efficiently diagnose conditions based on severity. It is known as the International Skin Tear Advisory Panel (ISTAP), and it breaks down severity into:
Type 1: No Skin Loss. A clinician can reposition the skin flap to successfully cover the entire wound bed.
Type 2: Partial Flap Loss. There has been partial tissue loss, preventing clinicians from successfully repositioning the skin flap to cover the entire wound bed.
Type 3: Total Flap Loss. In this phase, the skin flap is completely absent. The entire wound bed is exposed, and clinicians must prepare for secondary healing.
The treatment of skin tears is a safe, effective, and straightforward process. Most importantly, if possible, the physician will attempt to preserve the existing skin flap, minimize additional trauma, and maintain an optimal healing environment.
Below, we will discuss how to treat thin-skin wounds in elderly patients, including skin tears. This information is valuable whether you are a caregiver or caring for your own wound.
How to Treat Thin Skin Wounds in Elderly Individuals
Step 1: Gentle Cleansing
The proper cleansing agents make all the difference in how a wound heals. For example, it’s crucial to avoid harsh antiseptics as they can have negative effects on fibroblasts. Instead, use mild pH-balanced cleansing agents, warm water, saline solution, and any prescribed antimicrobial treatments.
Additionally, technique matters just as much as proper cleansing agents. With fragile elderly skin, it’s crucial to avoid harsh scrubbing. This can potentially damage surrounding skin or an existing wound bed, leading to slower healing or worsened injuries. The goal is to gently remove any debris and bacteria without disrupting healthy tissue.
Step 2: Bleeding Control
If you are experiencing a bleeding wound, apply gentle pressure using soft, sterile, and non-abrasive cloths. The bleeding should stop within 5–15 minutes of direct pressure. Additionally, while you may feel it's appropriate to apply adherent dressings (such as bandages) to a minor wound, avoid doing so unless directed by a clinician.
For fragile, thin skin, removing adhesive bandages can result in skin tears. Most importantly, bleeding control should be slow and precise, ensuring it doesn’t result in further trauma.
Related: Skin Prep for Wound Care: Best Practices for Proper Healing
Step 3: Wound Protection
Non-adherent dressings and soft wraps are excellent tools for protecting wounds. These materials will shield the wound bed from friction and contamination while simultaneously minimizing the risk of re-injury.
For fragile elderly skin, foam dressings are the safest and most ideal choice. Research even suggests that silicone foam dressings treat skin tears 50% faster. More specifically, they’re extremely effective at protecting fragile skin, providing cushioning, and offering pain-free removal. Additionally, they manage wound exudate without macerating the surrounding periwound skin.
Related: Types of Foam Dressings and When to Use Each One
Step 4: Moist Wound Healing
For the longest time, many were told that letting a wound “air out” is the most effective way to treat and heal it. Fortunately, due to modern research, we now know that a moist wound environment results in faster, better-quality recovery. A moist—not wet—environment improves growth factors, facilitates autolytic debridement, and reduces pain.
Essentially, the proper environment supports the body’s natural healing process. This is another reason why wound dressings are essential. In addition to protecting wounds, they maintain a moist environment by balancing fluid absorption with moisture retention.
Step 4: Monitoring Wound Continuously
Throughout the healing process, whether you’re overseeing the management of skin tears or treating minor lacerations, continuous monitoring is essential. Keep a close eye out for signs of infection, including redness, warmth, swelling, drainage, or odor. Ultimately, early detection is critical for reducing the risk of infection and preventing escalation.
And, most importantly, remember: you do not have to go through treatment alone. Qualified wound care specialists are here to help treat, heal, and monitor elderly skin wounds. And at Royal Wound Care, we offer mobile wound care, home health care, and in-clinic care to help you access treatment wherever you are in recovery.
Related: When to See a Wound Care Specialist
Thoughtful, proactive wound care allows caregivers and individuals to support better healing outcomes in elderly patients.
While skin structure varies with age, wound care procedures generally remain the same. Proper strategies, as in many other settings, prioritize reducing the risk of infection, improving comfort, and enhancing quality of life. However, for those with thin, fragile skin, technique matters just as much as simple steps. Remain gentle, effective, and consistent. And, most importantly, continue monitoring to ensure proper healing and early identification of complications.
At Royal Wound Care, we don’t just treat individual wounds—we treat patients as a whole. Our highly specialized team considers lifestyle factors, pre-existing conditions, and risk factors to create tailored, personalized plans. If you or a loved one is managing elderly wounds, we encourage you to contact Royal Wound Care today!
Additionally, our mission doesn’t stop at providing consistent care. SNFs and independent nurses can benefit from our unique educational opportunities and professional partnerships. From hands-on learning to expert-level precision, experience firsthand what improved outcomes, avoidable hospitalizations, and lower facility costs truly feel like. Accessible, patient-led treatment starts here!
To learn more, visit what Royal Wound Care partners experience.
